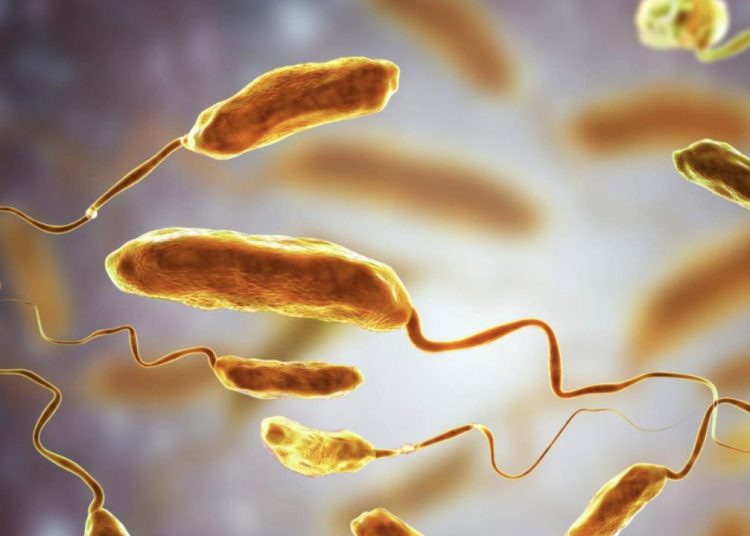
Five people have died this year in the Tampa Bay area from “flesh-eating bacteria.” The pathogen, known as Vibrio vulnificus, is found naturally in warm, brackish seawater. So far in 2023, a total of 25 cases have been reported in the state of Florida.
Although the infection is rare, it is especially dangerous for those who have open wounds or eat raw shellfish, such as oysters. The bacteria can be fatal in 50% of cases if it enters the bloodstream. To prevent infections by this microorganism it is recommended to avoid the sea if there are cuts in the skin, to cook shellfish properly, and wear protective clothing when handling them.
Vibrio vulnificus is a bacillus that belongs to the genus Vibrio, the same as Vibrio cholerae, the causative agent of cholera, to which we recently dedicated an article. It is a bacteria that can survive in environments without oxygen, is rod-shaped and withstands high alkalinities. It is especially dangerous for people with compromised immune systems such as diabetics, steroid users, cancer patients…
This pathogen can cause three manifestations. The first, when contaminated food is ingested, where gastrointestinal symptoms such as diarrhea, vomiting, abdominal pain, and fever may appear. Second, the most serious, when the bacteria is able to reach the blood and is clinically characterized by the presence of fever, chills, decreased blood pressure, and, in severe cases, septic shock. This manifestation has a close to 50% mortality. Finally, when it infects open wounds, it is capable of generating soft tissue infections, which can potentially be disfiguring and, in many cases, fatal.
Flesh-eating bacteria?
When you read the term “flesh-eating bacteria,” you picture a germ that literally feeds on human flesh. Does that really happen? No, Vibrio vulnificus and other bacteria do not eat flesh. However, they produce a manifestation that may lead one to think that they do.
These are the so-called necrotizing soft tissue infections. These manifestations are characterized by appearing in the extremities and the perineal region. It is important to remember that the perineum is the part of the body that gives rise to the pelvic floor, where the anus and external genital organs are located. It is made up of muscles and ligaments that simulate the shape of a diamond.
When a bacterial infection occurs in these areas, both due to the effect of toxins and other complex mechanisms, occlusion of the small blood vessels that go under the skin and subcutaneous tissue occurs. This occlusion causes heart attacks and necrosis (death) of these tissues. This, in turn, facilitates the growth of these bacteria, which are capable of living in anaerobic conditions, that is, without oxygen, permanently or not, as is the case with V. vulnificus. A vicious circle is then established in which more toxins are produced, more blood vessels are occluded, more tissue is necrotic (dying) and it gives the impression that the bacteria are “eating the flesh,” because all that dead or damaged tissue has to be removed (cut) surgically. Otherwise, almost certainly, it would cause the death of the patient.
Brief history of necrotizing soft tissue infections
The first description of this type of disease dates back to the 5th century BC, and was recorded by Hippocrates. Then, in 1871, the military surgeon Joseph Jones, during the American Civil War, made a detailed reference to the disease, which affected 2,642 soldiers with a close to 50% mortality, calling it “hospital gangrene,” as opposed to a classic manifestation called “gas gangrene,” which is characterized by the presence of gases in the necrotic area.
Later, in 1883, A. Fournier, a French doctor specializing in sexually transmitted diseases, published a detailed description of the necrotizing infection of the perineal region, which is currently known, in honor of this doctor, as “Fournier’s gangrene.” It was not until 1924 that the surgeon Frank L. Meleney established that the causal germ of most cases was Streptococcus, after isolating the bacteria in the blood culture of 20 patients in Beijing, coining the name “acute hemolytic streptococcal gangrene.”
Despite better knowledge of this disease and the availability of more efficient therapeutic tools, mortality from these conditions has hardly changed in recent years. But what structures are involved in this manifestation? Why are they called soft tissue infections? What are those “soft tissues”? What germs are involved?
Necrotizing soft tissue infections
Before continuing, we must stop and explain a little about what is meant by soft tissues and what are the structures that compose them. In this case, we are talking about the deepest layers of the skin and an important and little-known structure called the muscular fascia.
The skin is made up of three layers:
- Epidermis (outermost)
- Dermis (intermediate)
- Hypodermis (deeper)
For the purposes of this article, we will only refer to the last two. In the dermis are the sensory receptors, which allow the body to receive external stimuli and react to pressure, pain and temperature. There are also blood vessels, which provide the skin with the necessary oxygen and nutrients, and remove waste. Finally, we find different glands, such as the sebaceous glands, which produce skin oil, which prevents it from drying out. They are all over the body, except for the palms of the hands and the soles of the feet. The deepest layer of the skin is the hypodermis. This contains the fat cells, or adipose tissue, which insulate the body, help it to conserve heat, and constitute an important reserve of energy.
Immediately below the skin is the muscular fascia. This structure has among its functions to hold the muscles together and in the right place; separate them so they can work independently and provide a lubricated surface so they can move smoothly against each other.
Necrotizing soft tissue infections affect the dermis, hypodermis, and fascia, giving rise to conditions known as cellulitis, subcutaneous infection, and necrotic — or necrotizing — fasciitis, depending on the structures affected.
Although Vibrio vulnificus was the germ that gave rise to this article, it is the least frequent and important of those that usually cause these manifestations. The infections caused by it are classified into group or type III. Type I infections are those caused by more than one pathogen, known as “polymicrobial,” which generally occur in diabetic and immunosuppressed patients and usually generate gas, which is why they are reminiscent of “gas gangrene.” Finally, type II infections are produced by a single germ, generally streptococci or staphylococci. It is usually seen in younger patients, with a history of drug use, accidents, or recent surgeries.
Clinical manifestation and treatment
The main symptom of necrotizing soft tissue infections is severe pain. In patients with normal sensation, pain appears out of proportion to the magnitude of the lesions observed. The affected area is usually red, hot and swollen and turns pale quickly, which is a bad sign. Crackling blisters may appear, that is, they emit a sound reminiscent of plastic bags when squeezed in the hand. This occurs due to the presence of gas in the hypodermis.
At first, the muscles can be preserved, but as the condition progresses and deepens they will be affected. Patients appear seriously ill, with high fever, increased heart rate, altered mental status ranging from confusion to marked drowsiness, and decreased blood pressure.
Treatment of necrotizing soft tissue infection is surgical and should not be delayed. Due to the seriousness of this condition and the risk it entails for the patient’s life, the operation must be repeated every 1 or 2 days, with a larger incision. Sometimes it is necessary to amputate the affected limb. Intravenous antibiotics are adjuvant and usually include two or more drugs. It may be necessary to administer intravenous fluids in large volumes before and after surgery. Hyperbaric oxygen treatment may also be beneficial.
Gangrene and other Clostridium perfringens infections
A particular case due to its importance, within necrotizing soft tissue infections, refers to those produced by a germ called Clostridium perfringens. They usually appear several hours to days after a severe crushing injury to a limb or a penetrating injury that significantly damages tissue and creates anaerobic conditions, that is, in which there is no oxygen. Infection can also occur in surgical incisions.
Infections by this pathogen range from cellulitis, when the wound is superficial, to myositis, if it affects the muscles. Myositis is understood as muscle infection without necrosis (death) and is more common among drug users. Sometimes it can lead to a very serious condition that is “clostridial myonecrosis.” This manifestation is a classic of medicine and is popularly known as “gas gangrene.”
As the manifestation progresses, toxicity in the body increases, with an increase in heart rate, pallor and a decrease in blood pressure. Then organs and systems, such as the kidneys, begin to fail. It has the particularity that patients usually remain lucid until shortly before death.
Due to the rapid progression of this condition, surgical treatment is essential and is accompanied by the use of high doses of penicillin and other medications, as well as the use of hyperbaric oxygen, that is, at high pressures.